Reducing the Need for Benign Breast Biopsies using Ultrasound-guided Diffuse Optical Tomography
(R01CA228047)
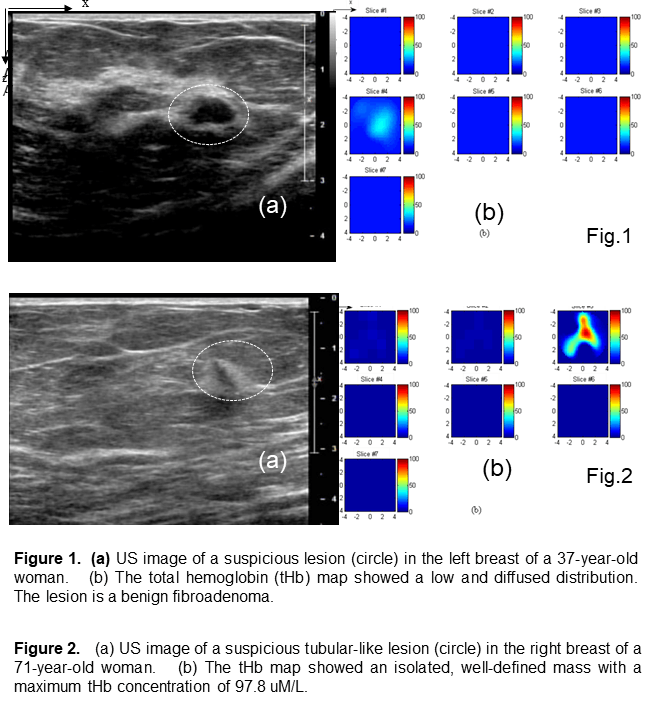
In current clinical practice, while the characteristics of malignant and benign breast lesions are well established by conventional imaging techniques, the overlapping appearances of malignant and benign lesions have prompted radiologists to recommend biopsy for most low and moderate risk breast lesions. As a result, in the United States, approximately one million image-guided breast biopsies are performed each year, with the majority of the lesions yielding benign results. This project will explore the potential of Ultrasound (US)-guided diffuse optical tomography (DOT) as an adjunct to US in a diagnostic setting, with the goal of reducing benign biopsies by providing additional lesion vascularity information. Three aims are: 1) Integrate a compact US-guided DOT system and automated data processing, data selection, and the reconstruction algorithms into a user friendly platform for on-site near-real-time diagnosis in the current standard-of-care clinical flow; 2) Prospectively assess the potential impact of adjunctive US-guided DOT in avoiding breast biopsy for patients with a breast abnormality of low or moderate suspiciousness on the basis of conventional breast imaging; and 3) Perform statistical analysis to validate the reduction of benign biopsy and potential of missing malignant lesions. The successful completion of the project may result in a paradigm shift in how we manage low risk benign lesions in current clinical practice and will reduce health care cost without compromising cancer detection sensitivity.
We are recruiting PhD students, postdoctoral fellows on research of robust DOT data preprocessing, finite element methods for modeling data distortion, robust imaging reconstruction, statistical and machine learning methods for data-adaptive imaging reconstruction.
Co-registered photoacoustic and ultrasound imaging for non-invasive ovarian cancer detection and characterization
(R01CA237664)
Current technologies (ultrasound, CT, MRI, PET, CA125 and physical exam) provide insufficient data to determine whether an ovary must be removed or is likely cancerous; therefore, a better method is needed to determine if ovarian tissue is malignant or benign. In this project, a new transvaginal imaging device optimized for ovarian cancer detection and diagnosis has been developed and validated from ex vivo and in vivo clinical studies. We have studied ovaries from both premenopausal and postmenopausal women with normal, abnormal and malignant ovarian tissue in an attempt to provide a more cost effective and accurate diagnostic technique to aid doctors and patients in determining the need for surgery. The successful completion of the project may provide a means to improve the current clinical practice; it will provide necessary technology to improve early ovarian cancer detection; and it will be an effective means to avoid surgery in most patients with a normal ovary.
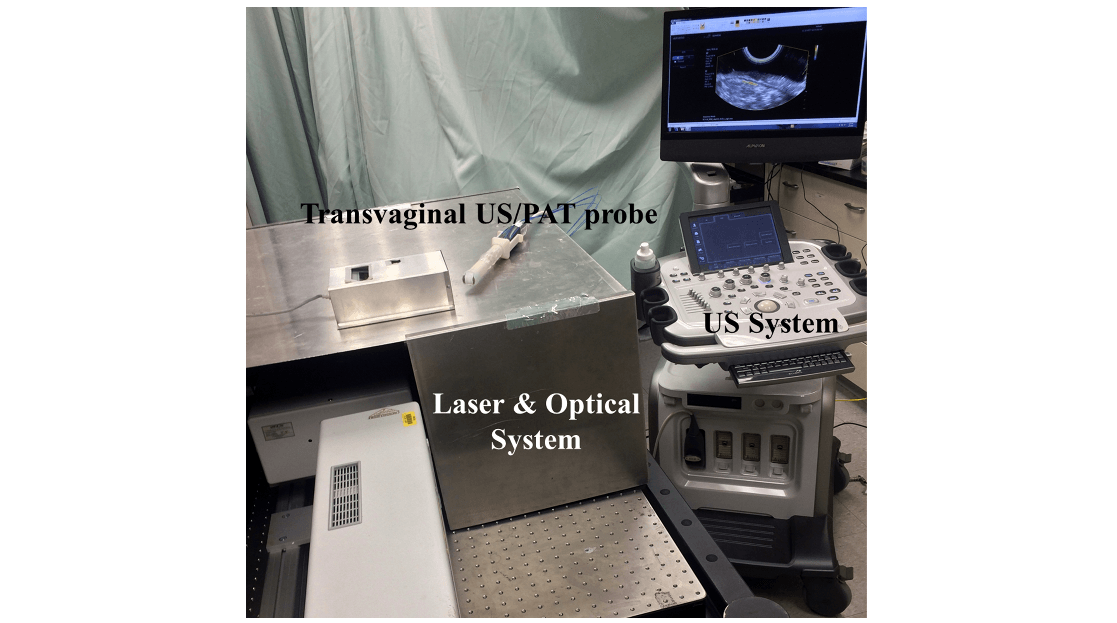
We are recruiting motivated PhD students and post docs on research of photoacoustic systems, experiments, photoacoustic imaging algorithms, methods of machine learning to distinguish malignant from benign lesions.
Optical and photoacoustic imaging for non-invasive diagnosis of colorectal cancer and assessment of colorectal cancer response to treatment
(The Foundation for Barnes-Jewish Hospital, NIBIB R01EB034398-01)
Colorectal cancer remains the 2nd most common malignancy diagnosed worldwide and accounts for over 100,000 new cases annually in the US. Current treatment methods typically involve surgical resection with selective use of radiation and chemotherapy depending on disease site and stage. Some of the greatest gains in survival, however, have come from aggressive endoscopic screening. However, several scenarios continue to complicate endoscopic surveillance: identification and assessment of flat neoplasia like sessile polyps and oncologic restaging following neoadjuvant therapy; these can harbor early cancers but remain difficult to identify with standard endoscopic techniques. Additionally, quantitative evaluation of the mucosa for residual rectal cancer after neoadjuvant treatment remains exceedingly difficult by flexible or rigid endoscopic technology.
We are developing, Optical Coherence Tomography (OCT), structured light, and photoacoustic microscopy techniques for non-invasive diagnosis and staging of colorectal cancers, and assessment of treatment response of colorectal cancers.